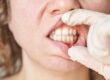
Dental implant surgery is considered one of the most successful restorative procedures in dentistry, but it is not completely free from complications. One of the most significant causes that may lead to dental implant failure is gum inflammation around dental implants. This inflammation may start with mild symptoms, but if not treated quickly and effectively, it can lead to complete implant loss. Early prevention and prompt intervention are just as important as choosing a skilled dentist.
What is gum inflammation in general?
Gingivitis often results from insufficient or improper cleaning with a toothbrush and dental floss. It can also result from medical conditions or the use of certain medications.
When inflamed, the gums become red, swollen, and bleed easily. Diagnosis is usually based on a dentist’s examination of the patient’s gums. Good oral hygiene, daily brushing, and proper nutrition help eliminate and prevent gingivitis. Mouthwash can also be beneficial in this regard.
Gingivitis is a very common condition in which the gums become red, swollen, and bleed easily. It may cause mild pain in early stages, or no noticeable pain at all. Untreated gingivitis may progress to periodontitis, a more severe condition that can ultimately lead to tooth loss.
What is gum inflammation around dental implants?
Peri-implant mucositis refers to an inflammatory condition affecting the soft tissues surrounding the implant without initially affecting the bone. As the condition progresses, it may develop into peri-implantitis, which causes bone loss around the implant and may lead to implant failure.
Causes of gum inflammation around dental implants
Bacterial causes: plaque and bacteria accumulation
The most common cause is bacterial infection resulting from plaque buildup around the implant. Lack of regular cleaning contributes to bacterial accumulation and irritation of surrounding tissues.
Mechanical causes: excessive pressure on the implant
If chewing forces are not properly distributed, excessive pressure may occur on the implant, damaging surrounding tissues and creating an environment for inflammation.
Health-related causes: diseases such as diabetes
Chronic diseases like diabetes reduce the body’s resistance to infection and slow healing, making patients more susceptible to gum inflammation around implants.
Behavioral causes: smoking and poor oral hygiene
Smoking negatively affects blood flow to soft tissues, and poor daily oral hygiene worsens inflammation around the implant.
Symptoms of gum inflammation around dental implants
- Redness and swelling of the gums: early signs of a problem around the implant
- Bleeding during brushing: repeated gum bleeding indicates inflammation
- Pain or discomfort around the implant: especially during chewing or pressure
- Bad breath: caused by bacterial buildup and inflamed tissues
- Implant mobility (advanced cases): indicates bone loss and possible implant failure
- Gum abscess formation
- Movement and instability of the implant
- Swollen lymph nodes in the neck
- Implant loss (falling out)
- Gum recession
- Exposure of the implant screw
Accurate diagnosis
Clinical examination: dentist assesses gum color, swelling, and bleeding
X-rays: used to detect bone loss around the implant
Pocket depth measurement: using a periodontal probe to assess severity
Implant stability tests: to evaluate osseointegration and fixation
Treatment options for gum inflammation after dental implants
Treatment begins with a precise plan based on severity and tissue involvement:
Deep cleaning:
First step involves removing plaque and bacterial deposits using specialized instruments that do not damage the implant surface.
Laser therapy:
Used to eliminate bacteria in peri-implant pockets with high precision, reducing inflammation, pain, and bleeding.
Antibiotics (topical and oral):
Prescribed in case of bacterial infection, either locally applied or taken orally under strict dental supervision.
Antiseptic mouthwash:
Chlorhexidine mouthwash is recommended to reduce bacterial growth, used for a limited period to avoid staining or taste alteration.
Gum surgery:
In advanced cases, surgical removal of infected tissue and deep cleaning around the implant may be required.
Implant replacement:
If the implant is severely affected and mobile, removal may be necessary followed by healing and reassessment for a new implant.
Bone and gum grafting:
Used to restore lost bone or soft tissue, improving implant stability and aesthetics.
Latest technologies in treating peri-implant inflammation
With the rapid advancements in dental implant technology, new techniques have emerged to improve treatment outcomes and reduce the risk of implant failure. Here are some of the most important techniques:
1- PRP (Platelet-Rich Plasma):
This technique involves taking a blood sample from the patient and then separating the platelet-rich plasma. This plasma is then injected directly into the tissues surrounding the implant, stimulating better healing of the gums and bone and reducing inflammation.
This method is safe because it uses the patient’s own cells and is increasingly used to treat peri-implantitis and support implant stability.
2- Stem cell therapy:
This is a promising technique, especially in severe cases where there has been significant bone or soft tissue loss. It involves extracting stem cells from specific tissues in the body and then reimplanting them in the area surrounding the dental implant to stimulate natural tissue regeneration.
Although it is still in the research phase in some countries, it shows positive results in cases of advanced peri-implantitis.
3- Nanotechnology cleaning techniques:
Ultrasonic cleaning tools using nanotechnology are used to reach the most delicate areas around the implant and remove microscopic bacteria without damaging the implant surface. This reduces the chances of recurrent infection and helps maintain the implant properly.
This technique is particularly beneficial in cases that do not respond to traditional treatment and reduces the need for surgical intervention.
Comprehensive prevention plan
Daily care routine:
- Use a soft toothbrush designed for implants twice to three times daily
- Use water flosser or interdental brushes for hard-to-reach areas
- Use non-abrasive toothpaste to protect implant surfaces
- Use dentist-recommended antiseptic mouthwash (alcohol-free preferred)
Regular dental visits:
- Visit every 4–6 months for implant evaluation
- Assess implant stability and gum health
- Take periodic X-rays to monitor bone condition
Conclusion
Gum inflammation around dental implants is not a minor issue—it can lead to permanent implant failure if not managed properly. Maintaining oral hygiene and regular dental follow-ups are key to successful implant longevity. Respond quickly to any symptoms and follow your dentist’s instructions carefully. Prevention starts with a small step, but its impact lasts a lifetime.
FAQs
What is the difference between peri-implant mucositis and peri-implantitis?
Peri-implant mucositis is an early warning stage involving only gum inflammation and is reversible with proper cleaning. If ignored, it progresses to peri-implantitis, where infection reaches the bone, causing bone loss and implant failure.
What are the warning signs of implant infection?
Early signs include bleeding gums, bad taste, redness, swelling, and in advanced cases, implant mobility. Pain is usually a late symptom, so regular check-ups are essential.
Can an infected dental implant be saved?
Yes, if detected early. Laser therapy and regenerative treatments such as bone grafting can often save the implant by removing bacterial biofilm and restoring lost bone.
How do I properly clean dental implants?
Use interdental brushes with plastic coating and a water flosser daily. Avoid metal tools that may scratch the implant surface, as this increases bacterial attachment risk.