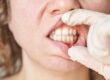
Tooth rot (also referred to as severe dental decay) is one of the most common reasons for visiting a dentist. Rotten teeth are painful and also embarrassing, especially if they are located at the front of the mouth. However, fixing the problem may not be as difficult or expensive as you think. If your teeth are severely affected by tooth decay, schedule an appointment with your dentist for proper evaluation and discussion of available treatment options.
Tooth rot is a serious condition that begins as simple tooth decay and may progress to involve the dentin, gums, and even the jawbone and nerves. If tooth decay is left untreated, it can worsen and may lead to tooth loss or long-term health complications.
What is a tooth made of and what are its layers?
A natural tooth is made up of protective layers:
- Enamel: the outermost layer of the tooth. It is semi-transparent and reflects the color of the underlying layer.
- Dentin: the second layer, a strong structure that protects the tooth from external harmful factors such as bacteria.
- Dental pulp (nerve): the innermost layer of the tooth. It represents the “life” of the tooth, containing blood supply and nerve tissue.
What is tooth pulp rot?
With frequent consumption of sugary foods or poor oral hygiene, an unwanted process occurs: bacteria produce acidic substances with sugars, which dissolve the protective layers of the tooth such as enamel and dentin. Gradually, the tooth begins to erode, and a dark cavity appears—this is known as dental caries.
If this tooth decay spreads quickly inside the tooth, the cavity becomes larger, darker, and may turn black. This is what is referred to as tooth rot.
Tooth rot does not stop at these layers; it may reach the dental pulp, causing nerve death. This is an advanced stage of tooth decay that is often difficult or even impossible to treat in many cases.
Causes of tooth rot
- Poor oral hygiene: relying only on a toothbrush without floss or mouthwash leads to plaque buildup and enamel breakdown.
- Excess sugar and starch intake: sugars are the main fuel for decay-causing bacteria, especially when food remains on teeth for long periods.
- Chronic dry mouth: due to medications or medical conditions, reducing saliva that protects the teeth.
- Age and medical conditions: such as acid reflux, vitamin D deficiency, and smoking—all increasing susceptibility to tooth decay.
Stages of Tooth Rot
Tooth rot develops gradually as a result of untreated progression of tooth decay. It develops through three main stages:
Stage 1 – Superficial tooth decay
In this stage, oral bacteria—feeding on leftover sugary and starchy foods—begin producing acids that attack the tooth enamel, the hard outer protective layer of the tooth.
At first, white chalky spots or faint lines appear on the outer surface of the tooth. These are early signs of mineral loss from the enamel.
At this stage, the patient usually does not feel pain, and this stage can be reversed using fluoride toothpaste and a therapeutic mouthwash under the supervision of a dentist.
Stage 2 – Tooth decay reaching the dentin
When the enamel loses its resistance, acids move to the next layer, the dentin, which contains microscopic tubules connected to the tooth nerve.
Since dentin is softer than enamel, tooth decay spreads more quickly. At this point, the patient begins to experience tooth sensitivity, especially when consuming hot, cold, or sugary foods.
The tooth may also start to change color into shades of yellow or brown, and bad breath may begin to appear.
Stage 3 – Advanced tooth rot
At this serious stage, the decay reaches the dental pulp, where the nerves and blood vessels are located. Bacteria begin invading the living tissues inside the tooth, causing severe inflammation or abscess formation.
The patient experiences intense, persistent pain that may radiate to the face, ear, or neck.
The tooth may become slightly mobile, and swelling or puffiness may appear in the surrounding gum tissue.
In many cases, the breath becomes extremely foul, and signs of infection or even fever may develop if the inflammation spreads.
In some cases, the nerve inside the tooth dies, and the severe pain turns into numbness. This may give the false impression that the problem has resolved, while internal damage continues and the infection may spread to the surrounding bone or adjacent teeth.
Symptoms of tooth rot
Imagine food that starts to rot—the first signs are color change and bad smell. The same happens with teeth. They turn darker or even black, with bad breath and embarrassment when smiling.
There is also increased sensitivity and severe pain due to loss of protective layers, which exposes the dental pulp (nerve).
In advanced cases, infection may lead to abscess formation, swelling in the gums, jaw, or face, requiring urgent dental treatment.
Modern treatment methods for tooth rot
With the advancement of dentistry, treating tooth rot is no longer limited to traditional dental fillings or tooth extraction only. Instead, multiple options are now available depending on the degree of damage and the extent of tooth rot inside the tooth or into the surrounding tissues. Here are the details:
1. Conservative treatments
These treatments aim to save the tooth if tooth rot has not reached a very advanced stage:
Self-healing fillings:
The latest types of dental fillings that do not only fill the cavity, but also release materials that help prevent bacterial growth and promote remineralization of tooth enamel. They can also release fluoride gradually to protect the adjacent tooth from tooth decay.
Laser root canal treatment:
When tooth rot reaches the dental pulp, dentists use laser technology to clean the root canals and disinfect them with higher precision compared to traditional instruments. The laser reduces pain, speeds up healing, and reduces the chances of recurrent infection.
Preventive crowns:
When the tooth structure is partially damaged, a ceramic or zirconia dental crown can be placed to fully cover the tooth and protect it from further breakdown, while preserving the root and nerve if they are still healthy.
2. Surgical treatments
These are used when the tooth is severely rotten and cannot be saved with fillings or root canal treatment:
Tooth extraction:
If the tooth is completely damaged and causing repeated infections, it is removed to prevent the spread of infection, and later replaced with a dental bridge or dental implant.
Immediate dental implants:
After extraction, in some cases an immediate dental implant can be placed in the same session if there is no active infection. This procedure reduces the number of visits and preserves the shape of the gums and bone.
Bone grafting:
If severe tooth rot causes erosion in the jawbone, bone grafting can be performed to replace the lost bone and ensure stability for future dental implants.
3. Advanced technologies
Stem cell therapy:
Stem cell therapy is one of the most important modern innovations, where regenerative cells are used to stimulate repair and regenerate damaged tissues inside the dental pulp or around the root. Although still under research, early results are promising, especially in treating chronic inflammation.
Nanotechnology:
Nanomaterials are used in the production of dental fillings and dental crowns to help kill bacteria and prevent plaque formation again, which increases the lifespan of dental restorations and prevents recurrence of tooth rot.
Bioactive materials:
New materials that stimulate natural healing in the body and bond more strongly to the tooth, improving both functional and aesthetic outcomes.
What are the steps for treating tooth rot?
It is logical in treating this type of advanced tooth decay or what is called a rotten tooth that the treatment should depend on the level of damage that has affected the tooth.
If the damage affects only the outer layers of the tooth and the pulp is still alive, your dentist can remove this rot in a way that preserves the remaining healthy part of the affected tooth, then fill this cavity with cosmetic tooth-colored dental fillings. The tooth may also need additional support if the remaining structure is minimal, using fixed dental restorations such as dental crowns.
However, if this tooth rot results in the destruction of a large part of the pulp or the tooth nerve, the dentist needs to remove the damaged nerve, disinfect the root canals, and fill them with materials that prevent the occurrence of inflammation in the nerve area again. In this case, the tooth needs external protection such as a crown to prevent it from breaking.
Finally, if this damage has destroyed a large part of the tooth, it may unfortunately need extraction and replacement with fixed dental restorations, removable dentures, or dental implants.
Prevention tips for tooth rot
- Daily care routine: Brush your teeth twice daily, use dental floss and antiseptic mouthwash, and attend regular dental check-ups.
- Healthy dietary habits: Avoid excessive sugar intake and maintain moderate consumption of hard foods that help clean teeth naturally.
- Regular check-ups: Visiting the dentist every 6–12 months is essential for early detection of any tooth decay or changes in tooth color or structure.
- Important note: Avoid using a treated tooth for hard foods, as it may fracture due to loss of a significant portion of its natural structure.
Conclusion
Tooth rot is not just advanced tooth decay, but a medical condition that can affect the entire oral health if not treated in time. Symptoms may start simple, such as tooth discoloration or bad breath, but may progress to chronic pain, repeated infections, or even complete tooth loss.
Thanks to advancements in dentistry, it is now possible to treat tooth rot with precise and effective methods, starting from preventive fillings, passing through advanced root canal therapy, and even modern dental implants. However, early detection and regular follow-up with a dentist remain the key factors in avoiding complications and saving natural teeth before it is too late.
At Wonders dentistry, we provide you with a specialized team and the latest diagnostic and treatment equipment to deliver comprehensive care for tooth rot cases, with the highest standards of sterilization and quality, and with treatment plans tailored precisely to your individual case.
Restore your smile with confidence… take your first step with us at Wonders dentistry. Book your consultation now.
FAQs
Does tooth rot necessarily mean the tooth must be extracted immediately?
Absolutely not. Although the term “tooth rot” sounds alarming, modern dentistry focuses on preserving teeth. If the root structure is still strong, microscopic root canal treatment can be performed to remove damaged tissues and fully disinfect the canals. The tooth is then reinforced with a high-strength zirconia crown, allowing it to function normally again.
Why does pain in a rotten tooth sometimes stop suddenly?
This is usually a warning sign, not recovery. Sudden pain relief typically means that the tooth nerve has completely died (necrosis). The infection has not disappeared; instead, it may have started spreading from inside the tooth to the surrounding bone, which can lead to a dental abscess. It is essential to visit Wonders dentistry immediately to clean the infection before it affects the jawbone and overall health.
Can one rotten tooth cause tooth decay in adjacent healthy teeth?
Yes, but indirectly. Tooth rot is caused by heavy bacterial activity (biofilm). A rotten tooth increases the concentration of harmful bacteria in saliva, creating an environment that attacks the enamel of neighboring teeth. Treating the “source of infection” at our clinic helps reduce the bacterial load and protects the rest of your teeth from infection.
How is bad breath caused by tooth rot eliminated?
This odor is caused by gases released by bacteria during the breakdown of organic tissues inside the tooth. The only effective solution is to remove the source of infection and disinfect the tooth using a proper clinical protocol. Once the canals are cleaned, disinfected, and sealed with fillings and biocompatible restorations, the bad smell disappears immediately because the root cause has been eliminated.